A. Musculoskeletal back pain
Musculoskeletal pain refers to discomfort and pain that is generated by the bones, ligaments, tendons, and/or muscles of the spine. One of the most common causes of pain in the back and neck is muscular strain. Overuse of the muscles of the spine is common. These muscles are part of the axial skeleton (as opposed to the appendicular skeleton which refers to the limbs) and they are constantly in use supporting our weight. They are typically working even when we are sitting or lying down. The musculature of the axial skeleton has a different control system located in the cerebellum of the brain. The constant demand on these muscles makes it difficult to rest them and therefore difficult to control pain generated by them. Overuse and strain of the muscles can easily cause pain that lasts for hours to days. Without appropriate treatment, it can get worse rather than better. Additionally, muscle spasms can developed which can cause episodic severe pain. Other causes of musculoskeletal pain include degeneration of the disks of the spine, and degeneration of the facet joints of the spine. These can be considered a form of arthritis, similar to osteoarthritis seen in many parts of the body. Degenerative disc disease and facet arthritis can occur in isolation, but are often associated with muscle pain as well. Musculoskeletal pain is typically described as dull, aching, throbbing, and/or stabbing. It can often be improved with typical pain medications. There are many other causes of spine pain such as fractures and tumors, but those are generally addressed as separate pathologies.
B. Nerve pain
The purpose of the spine is to support the body, but it also houses many nerves as they pass from the brain to the periphery of the body. These nerves include the spinal cord which resides in the neck and upper back and nerve roots which branch from the spinal cord at each level innervating the arms, trunk, and legs. When these nerves are compressed, or pinched, they generate pain in the area to which they provide innervation as well as in the spine itself. For instance, a pinched nerve root in the neck will cause pain in the portion of the arm to which that nerve travels. Similarly, a compressed nerve in the low back will cause pain in the leg or foot. This pain may be accompanied by altered sensation (numbness and/or tingling) and weakness of the muscles served by that nerve. Nerve pain often has a tingling or burning quality and is difficult to treat with typical pain medications.
II. Treatment of spine pain The initial management of almost all pain from the spine is conservative (nonoperative). It starts with simple, low risk strategies focused on improving pain, increasing activity, and restoring normal functional levels. These strategies are generally initiated by a primary care provider and include medication, activity modification, and referral to physical therapy. If initial therapeutic modalities are not successful, patients may be prescribed different medications and they may be referred to a pain specialist for injections. Finally, surgery may be considered in patients with severe pain that is limiting activities of daily living. They must be acceptable medical candidates for surgery, and there must be pathology on imaging studies that correlates with their pain syndrome that can be addressed with surgical intervention. Surgical intervention in the neck and back for neck and back pain without nerve pain is somewhat rare.
The following are some therapeutic modalities for treating spine pain. While each may be successfully used in isolation, they are much more successful when used together as part of a comprehensive, coordinated program.
1. Medication
NSAIDs (non-steroidal anti0inflammatory medications) This group of medications includes ibuprofen (Motrin, Advil) and naproxen (Aleve) which are available over-the-counter. There are also a number of NSAIDs that are available by prescription. These medications work by inhibiting a pathway that promotes inflammation and pain. These medications can be very helpful when dealing with musculoskeletal pain. They do have several drawbacks as they can cause gastrointestinal problems, kidney damage, and promote bleeding. When using these medications, when should adhere to the recommendations on the packaging or from the prescribing provider.
Corticosteroids
This is a group of powerful anti-inflammatory medications. They can be used to treat musculoskeletal as well as nerve pain. When used at high doses for an extended time, they can have significant side effects. Therefore, the most common use is a short course which starts at a high dose and rapidly tapers off. This group of medications includes prednisone, dexamethasone, and methylprednisolone (Medrol Dose Pack) among many others.
Acetaminophen
Acetaminophen (Tylenol) is probably the most common pain medication. It is a safe and effective medication that can be used alone or with other medications.
Muscle relaxants
This group of medications is helpful in treating musculoskeletal spine pain. They can be particularly effective when there is a complaint of muscle spasms. The primary drawback of muscle relaxants is sedation. A few of the more common muscle relaxing medications include cyclobenzaprine (Flexeril), methocarbamol (Robaxin), tizanidine (Zanaflex), metaxalone (Skelaxin). Baclofen and Soma are also muscle relaxants, but they are rarely used in the modern era.
Nerve modulating medication
This group includes gabapentin (Neurontin) and pregabalin (Lyrica). Both of these medications worked by mimicking the inhibitory neurotransmitter, GABA, reducing pain signaling at the level of the spinal cord and brain. As these medications work on the nerves themselves, they are often felt to be more effective in treating nerve pain. These medications can also be sedating.
Antidepressants
This group of medications works by altering the balance of neurotransmitters in the brain-typically serotonin and norepinephrine. This alteration of brain chemistry can lead to reduced perception of pain. They may have the added benefit of treating symptoms of depression and anxiety as well as pain; some may be effective in helping with quitting smoking as well.
Opioids
Opioid pain medications make a large class of drugs that all work by stimulating opioid receptors located in the brain and spinal cord. Stimulation of these receptors can block pain and cause euphoria or a "high" sensation. Over the last several decades, the medical community has realized that these medications can quickly lead to physiologic dependence and addiction, and that due to the body's up-regulation of opioid receptors, leads to a loss of effectiveness in treating pain. Additionally, super-therapeutic doses of these medications (over-dose) can lead to respiratory arrest and death. These medications are therefore most useful in treating severe, acute pain such as after surgery. They are carefully controlled by the DEA and should be weaned as quickly as possible.
Cannabinoids
Cannabinoids are a group of chemicals (medications) that are derived from the cannabis plant. The two main chemicals that have been made available are tetrahydrocannabinol (THC) and cannabidiol (CBD). THC has psychoactive effects and is listed by the DEA as a Schedule I substance (drug of abuse), and is therefore illegal according to the federal government. However, many states have adopted the use of medical marijuana. The medical use of THC is restricted to those who have obtained appropriate permission. Its use to treat pain should be under the direction of a medical professional and should not be inhaled (smoked or vaped). CBD is not well understood, but appears to be have anti-inflammatory properties. Both TCH and CBD have been used to treat pain, but there is no clear scientific evidence of effectiveness.
2. Physical therapy Physical therapy as a branch of medicine dedicated to reducing pain and improving function using physical methods rather than drugs or surgery. Common modalities include stretching, exercise, massage, and heat application. Treatment is delivered by physical therapist. In treating spine pain, therapy, commonly includes exercises for stretching and strengthening the muscles of the spine and abdomen to provide greater core strength. The therapy must also focus on posture and proper body mechanics so that the muscles of the spine can be used and strengthened in a manner that does not cause additional spine pain. Physical therapy of the spine uses modalities listed above and may also include spinal traction.
If traditional physical therapy is unsuccessful, other similar modalities may be appropriate. These include: Aquatic therapy. Physical therapy is performed in a pool. The weight of the body is buoyed up by the water, and the water additionally provides gentle resistance to movement improving many exercises.
Mechanical diagnosis and therapy (MDT, formerly called the McKenzie method of physical therapy). This method focuses on techniques of spinal extension used to centralize pain.
Chiropractics. This is a system of complementary medicine based on manipulative treatment of misaligned joints of the spine used to treat pain. Any aggressive manipulations of the spine should be avoided.
Massage. Manual manipulation of the muscles of the spine, shoulder and pelvic girdles can relax strained muscles and relieve spine pain.
Acupuncture. A system of complementary medicine derived from Eastern medicine. It uses small needles placed into the skin to relieve pain
3. Supportive and Assistive devices
Back Brace
Lifting belt. A supportive belt that is worn around the waist. They are available over-the-counter, vary in construction, and vary in price (often starting around $20). They typically provide less support than a lumbar orthotic (see below), allowing more range of motion, but still encouraging improved body mechanics and posture. One common band is Copper Fit. Others can be found at stores like Home Depot ( Safe Handler Lifting Support Weight Belt in Black-BLSH-ES-2LB - The Home Depot).
Lumbar orthotic brace. A medical back brace that requires a prescription to be dispensed. They are rigid, typically made with a plastic core and a padded nylon covering with hook-and-loop closure. The classic design is made of custom, thermo-molded plastic and is typically called a “clam shell brace.” More common recently is a one-size-fits-all, fully adjustable brace. An orthotic brace that covers only the low back is called a Lumbo-Sacral Orthotic brace or (LSO); if it extends to the chest, is is a Thoraco-Lumbo-Sacral brace (TLSO). A widely used example is the Aspen Horizon LSO. These braces provide exceptional support and can be adjusted for sitting, standing, or weight loss and are relatively low cost and immediate availability. The improved support helps the wearer improve or restore lumbar lordosis and maintain appropriate posture and use acceptably body mechanics. Lumbar orthotics are generally reserved for patients with defined pathology of the back including fracture or malalignment and are often used postoperatively.

Neck Brace
Soft cervical collar. A soft, foam collar that is worn around the neck to provide minimal support for comfort. They are widely available over-the-counter at most pharmacies for a low cost.

Hard cervical collar. A medical neck brace that requires a prescription to be dispensed. They are rigid, typically made with a plastic core covered with soft pads. They are typically used to treat spinal fractures and may be used perioperatively to provide rigid support of the neck. Common brands include Aspen, Miami-J, or Philadelphia braces.

Traction devices
Cervical home traction device. A device that is used to apply traction to the cervical spine. Traction is a force that pulls the head away from the body (opposite is compression where the head would be pushed into the body). Gentle traction in line with the spine is safe in most cases, and can be applied relatively easily to the neck. One type of system pulls weight of the head off of the shoulders using a chin strap and pulley system. A less cumbersome and inexpensive option is an inflatable device that can be found on most on-line shopping forums (e.g. Amazon). Traction applied to the neck relieves the bones of the spine of the weight of the head allowing the discs, facet joints, and muscles of the neck to rest and recover. Please consult a medical professional before using such devices.

Lumbar traction. A device that applies traction to the back and trunk. There are multiple systems available that can be used to apply a gentle force that pulls the shoulders away from the hips. This takes at least a portion of the weight of the body off of the lumbar spine allowing the discs, facet joints, and muscles of the back to rest and recover. One example would be an inversion table. Please consult a medical professional before use of these devices.
Others
Walkers and canes. These devices can be used to stabilize a person while walking and can transmit some of the weight of the body from the spine to the arms. Rolling walkers have become very popular and some even provide a seat for intermittent rests. One draw-back is that they promote walking with a stooped (flexed) posture of the lumbar spine which may promote pain. They are available in medical supply stores, and insurance may pay a portion of the cost in appropriate setting with a prescription. Consultation with a medical professional is recommended before use of one of these devices.

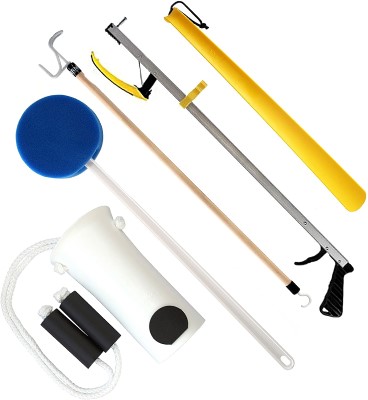
Hip kit. This is a clever collection of small devices that can be very helpful. There usually are six items in a hip kit: a sock aid, dressing stick, reacher, shoehorn, long-handled bath sponge, and elastic shoelaces. They are all used to limit one’s need to bend thus reducing strain on the spine and pain. These devices can be very helpful during a flair-up of back pain and also in the post-operative setting when a patient is restricted from bending.
4. Topical treatments
Topical treatments are medicines that are applied to the skin to relive pain. There are many types and some are outlined below. They are non-narcotic (do not contain controlled substances) and are generally available over-the-counter. They are typically applied directly to the skin over the area of pain. Consultation with a medical professional may be wise prior to use, and they should not be used if an allergy to any ingredient is present. They should not be used on a wound. Many preparations contain a mixture of medications that may have synergistic effects.
Menthol. This is a medication that causes the skin to feel cool and then warm, which distracts the nervous system from transmitting pain signals from the same area of the body. Menthol is an active ingredient in Biofreeze and Bengay.
Salicylates. This is a group of medicines that are similar in chemical structure and action to aspirin; a nonsteroidal anti-inflammatory (NSAID). They reduce inflammation and pain. This group includes Aspercreme and Bengay.
Lidocaine. Lidocaine is a medication that blocks nerve signals, including pain. It is a local anesthetic used to numb the skin for minor procedures including dental procedures. It can be applied to the skin in a cream or as a patch. The most common brand is Lidoderm patch, but it can also be found in other topical medications (Aspercreme with lidocaine, Icy Hot with lidocaine, etc.)
Diclofenac. An NSAID that works by blocking inflammation and pain. It is available as a gel both by prescription and over-the-counter. The brand name is Voltaren, but it is also available as a generic.
Capsaicin. This is a blocker of a neurotransmitter that is used to stop pain. It is derived from hot peppers and should be used very carefully – any medication that gets near the eye can cause severe pain and tearing (like pepper spray).
TENS (Transcutaneous Electrical Nerve Stimulation). TENS is a therapy that uses low voltage electrical current to provide pain relief. A TENS unit consists of a battery-powered device that delivers electrical impulses through electrodes placed on the surface of the skin. The electrodes are placed at or near nerves where the pain is located or at triggerred points. Electrical current from the TENS stimulates nerve cells. blocking the transmission of pain signals. reducing perception of pain. Stimulation may also raise the level of endorphins, which are the body's natural pain-killing chemical. The endorphins then block the pereption of pain. TENS units are available by prescription and may be recommended by a physical therapist, but are also available over-the-counter.
5. Spine injections
The purpose of a spine injection is generally two-fold. First is to treat pain, and second is to help identify the source of the pain. There are many types of spinal injections, a few are listed here.
Trigger point injection. In a TPI, a local anesthetic medication (a numbing medicine) is injected under the skin in an area that has been identified to be a focal site of pain and/or an area that triggers pain. They can provide rapid relief of pain and do not generally require special equipment.
Epidural steroid injection (EDSI). In this injection, a long needed is placed under the skin and in the space inside the spine that is under the bone, but outside the nerves (the epidural space). A corticosteroid medication, a very powerful anti-inflammatory, is then injected to reduce irritation and pain. This procedure is typically performed under fluoroscopic guidance (live x-ray pictures) by a pain specialist. It is typically indicated when symptoms and signs point to nerve irritation as the source of pain (ie. Radiculopathy). A successful injection can confirm that a patient’s pain is indeed from nerve irritation at a specific level of the spine.
Facet injection. The facet joint is one of a pain of joints found on each side of the back of the spine between two bones. Like any joint, it can become degenerated and arthritic, causing pain. There are many techniques, but one involves the injection of a numbing medicine (local anesthetic) adjacent to the joint to block its pain. A successful injection localizes the pain to that specific level and can then allow the direction of other therapies to that site.